 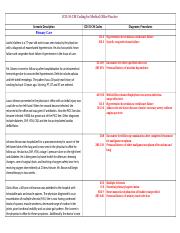
The child is diagnosed with an asthma exacerbation. During the examination, the provider notes wheezing with occasional cough. During the encounter, the patient’s mother mentions to the provider the patient has been coughing for the last couple of days and has a known diagnosis of asthma. In this case, the coder should assign code Z00.00 (encounter for general adult medical examination without abnormal findings) along with the appropriate codes for hypertension, hyperlipidemia, and diabetes.Įxample: A 3-year-old girl is seen for her well child exam. 
During the visit, the provider addressed his chronic conditions which include hypertension, hyperlipidemia, and diabetes, all of which are documented as stable and no adjustments in treatment are documented. If a stable, chronic condition(s) is addressed at the visit, an additional code may also be reported with the “without abnormal findings” code, if the documentation supports the condition(s) was addressed at the encounter.Įxample: A 56-year-old man is seen for his yearly physical exam. When a coder determines that a new or worsening chronic condition(s) was addressed and will be assigning a “with abnormal findings” code, an additional code(s) is required to identify the abnormal findings. If the documentation supports a new or exacerbated condition(s) were addressed, a “with abnormal finding” code should be reported. So, how can we easily decide which code to assign? Per Coding Clinic First Quarter 2016 “For the purpose of assigning codes from this category, an “abnormal finding” is a newly discovered condition, or a known/chronic condition that has increased in severity.” When documentation supports an additional condition is being addressed during a general examination encounter, it doesn’t automatically mean that a “with abnormal finding” code should be assigned.Ĭoders should carefully review the documentation to determine if the condition(s) being addressed are new or have increased in severity. When a provider addresses additional conditions at a general examination visit, usually referred to as a Well-Child or Adult Physical encounter, coders are often left to decide whether to assign a “with” or “without” abnormal findings code. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
